The way the term medical electronics is perceived by us has constantly evolved over time. At one time, it meant digital instruments to read one’s blood pressure or glucose levels, or large, Internet-connected meters that could be used by doctors to test and treat patients in remote locations (with the help of trained technical staff) or implantable devices like cardiac pacemakers. However, today the term has taken on whole new definitions, which are unimaginable and, even, unquantifiable.

From wearable devices that work with your mobile phone to monitor and convey your health condition to a physician, and devices that make sure you have your medicines and electronics built into your house’s walls to monitor your heart rate, to implantable devices that help your body work better, modern medical electronics is at the cusp of a new era of medical diagnosis and treatment. This is fuelled by trends like flexible, organic electronics, 3D printing and the Internet of Things (IoT).
Here we look at some futuristic research and development (R&D) in this space, which promise a lot of excitement and good health in the days to come.
Wearables and Big Data: A magical duo
Although it might seem as if the market is flooded with just fitness enhancers, some start-ups are already making some clinically-significant wearable devices, which have the potential to eventually bridge the gap between physicians and patients, making real-time medicine a reality.
Muse is a good example. It uses advanced sensor technology to fit the functioning of a clinical-grade electroencephalogram (EEG) into a beautiful and comfortable headband, which works hand-in-hand with an app to aid care givers an understanding and helping them out in conditions like attention deficit hyperactivity disorder (ADHD), anxiety and depression.
Another is Resound, an iPhone-connected hearing aid that can be customised according to location and situation.

A series of small devices being developed by CellScope, a spin-off from UC Berkeley, is also expected to bring advanced diagnostics home to common folks. Oto Home and Oto Clinic, for example, are small devices that fit onto the camera of a smartphone, enabling users to capture images of the ear’s membranes, to detect ear infections. The idea behind mobile phone microscopy, a concept pioneered by Fletcher Lab of UC Berkeley, is to develop small devices that add optics, illumination and hardware automation to the cameras of regular mobile phones and tablets, to create mobile microscopes and diagnostic solutions.
More on the anvil
The future holds many more such devices, as was seen at Elsevier’s 4th International Conference on Bio-Sensing Technology. One of the interesting technologies demonstrated at the event was a home diagnosis card developed in Sweden by Linköping University and Acreo. The device, the size of a credit card, takes a drop of blood or saliva as input from the user and gives diagnostic information on his or her phone. This information can help monitor diabetes, heart and kidney diseases and even cancer. Screen printing all electronics on the card makes it very cost-effective, too. It currently costs €5 each, but as volume picks up, it can be manufactured at €0.50 per piece.
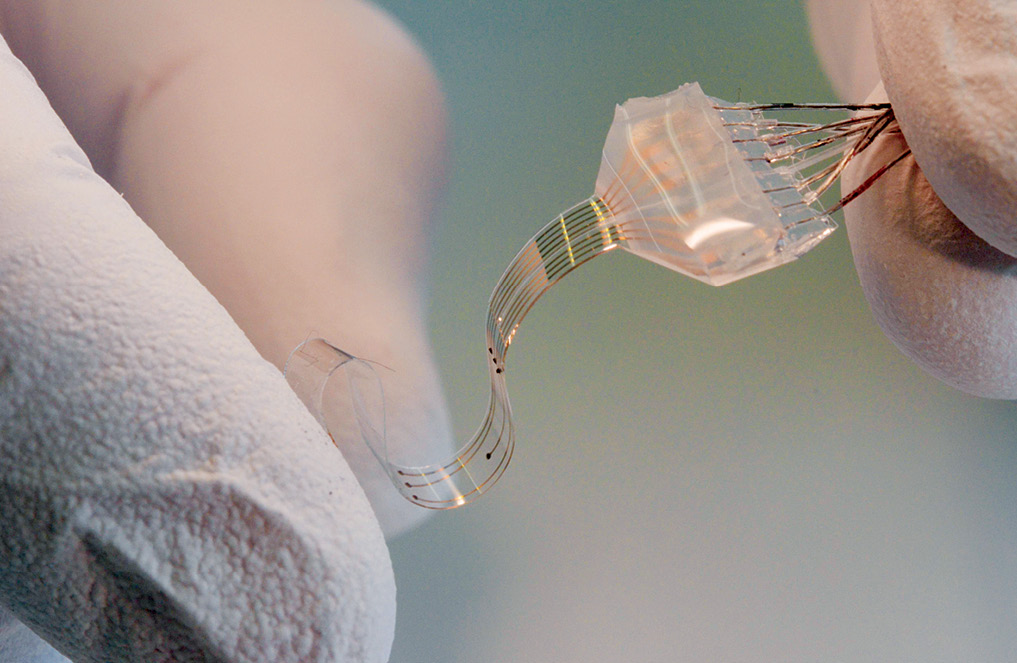
According to Elsevier’s press release on the event, “This means these have the potential to provide patients and doctors in developing countries with accessible, affordable medical tests. For example, the printed card could be made part of the packaging of antibiotics, helping determine which antibiotic would be best to treat a patient’s infection. Such printable devices could also be worn like plasters or contact lenses, transmitting information to mobile phones.”
Another recent development in this space is a type of e-skin developed by Suzhou Institute of Nano-Tech and Nano-Bionics, Chinese Academy of Sciences, China. Born of nanotechnology and flexible electronics, e-skin has the ability to detect changes in pressure, which can, in turn, be used to monitor blood pressure, heart rate and wrist pulse on real-time basis. The team has worked to make the sensor element very sensitive, while making the material very flexible. This they have done using carbon nanotubes and sheets of graphene only a few atoms thick.
Helping hand from Big Data
There are many more devices in the wearable cadre; however, the magic ingredient that will make these really useful is smart data analysis.
Dr Michael Docktor, a gastroenterologist at Boston Children’s Hospital, also clinical director of innovation and director of clinical mobile solutions, wrote in January in an article about CES 2015, “As these wearables become more of a clinical tool than merely a personal wellness device, data analytics and the ability to serve up meaningful, reliable and actionable data to one’s care team will be critical.”
Robots to the rescue
Carol Reiley, an experienced computer scientist and roboticist, spoke about future applications of robots in medical technology, at Bay Area Maker Faire 2015. The picture she painted was fantastic—of miniature robots that enter the body through natural openings like the mouth and perform surgeries inside. Some of these are devices like Pillcam that allow minimally-invasive imaging of a person’s colon, sensor-augmented surgical tools like the Intuitive Surgical Firefly system that injects a dye for fluorescent imaging to help identify tumours during surgery, augmented reality solutions that allow surgeons to look beneath the patient’s skin, robots that assist in therapeutic exercises and so on.
It is interesting to note that famous robotic contests like John Hopkins Robo Challenge have some quests that encourage children to solve problems similar to those experienced in the medical field. A challenge to build a robot that can spot a grape in Jello, for example, can be compared with finding a tumour in soft tissue.
Implants aplenty
When somebody says implant, you might be immediately reminded of devices like the pacemaker, which have been around for decades now. Now, take a look at these implants and you will realise the current generation is incomparable to medical electronics a decade back.
Dissolvable devices for drug delivery. Last year, researchers at Tufts University’s School of Engineering developed resorbable, wirelessly-controlled electronic implants made of silk and magnesium that could deliver heat treatment on a patient’s body tissues to treat bacterial infections and then safely dissolve. The device consisted of a serpentine resistor and a power-receiving coil made of magnesium deposited onto a silk-protein layer. The silk pocket protected the electronics and controlled the device’s dissolution time.
In a test on tissue infected with Staphylococcus aureus (S. aureus), devices were triggered through a wireless transmitter to administer two 10-minute heat treatments. The devices safely dissolved within two weeks. In a subsequent in-vitro lab experiment, another device was made to administer antibiotic ampicillin to kill E. coli and S. aureus.
According to Hu Tao, first author of the study, “The new wireless therapy devices are robust enough to survive mechanical handling during surgery but designed to harmlessly dissolve within minutes or weeks, depending on how the silk protein was processed.”
Helping paralysed people walk again. Historically, one of the biggest problems concerning implants has been the mechanical mismatch between soft tissue and stiff implants. For some, this can cause minor issues like inflammation, while for others, it might mean outright rejection by the body.
A team of multi-disciplinary experts in Switzerland has developed a soft, flexible implant called e-Dura, which mimics the shape and elasticity of dura mater, the protective membrane of the brain and spinal cord.
Armed with electrodes, interconnects and chemotrodes that can handle millions of cycles of mechanical stress, chemical injections and electrical stimulation pulses, the device enables those with a paralysed spinal cord to walk again. It is also capable of delivering electrical impulses and chemicals and even monitoring electrical signals from the brain in real-time. e-Dura, which has been tested successfully on lab rats, is now moving towards clinical trials. Because it has the same mechanical properties of dura mater, it avoids problems like inflammation and rejection, and can also remain in the body for a long time.
Magic cure for rheumatoid arthritis. British drug-maker GlaxoSmithKline recently demonstrated an implant capable of relieving patients of rheumatoid arthritis, a chronic condition that afflicts innumerable people across the world. The tiny device—the size of a small coin—is embedded into the neck of the patient, from where it influences the nervous system by sending electrical impulses into a major nerve that relays brain signals to the body’s major organs.
Firing such impulses for around three minutes a day has shown to reduce the amount of chemicals produced by the spleen, which is responsible for abnormal inflammation in the joints of people with rheumatoid arthritis.
The company is working to develop a smaller version of the device, and hopes that in the future, this ability to bring about a balance in the body can also help cure conditions like diabetes and asthma.
Medicine’s tryst with 3D printing is rather exciting
Imagine the day when doctors can print customised implants and medical devices for their patients, right on their desk! Well, that day is not too far off, considering some of the recent advancements in 3D printing.
Old World Labs (OWL), for example, has demonstrated two printers, MC-1 and MC-2, which use a process called stereolithography (SLA) to print objects, unlike most other current-generation 3D printers that use fused deposition modelling (FDM) technique.
In an SLA, lasers harden layers of liquid plastic or resin into 3D shapes. This can create much more detailed devices with a smoother finish as compared to FDM. OWL’s makers claim that their printers are even better than other SLA printers in the market, as these can print objects that are 200 times more accurate than objects created with other SLA printers.
The company is also exploring useful medical technology that can be printed with these machines. For example, one can print microfluidic devices to deliver drugs to cancer patients. These devices are highly detailed, with tiny channels that circulate prescription drugs into a patient’s body.
It is also possible to print bio-resorbable tissue scaffolds with resins (pending FDA approval), for cartilage-replacement surgeries. The tissue scaffolds, injected with stem cells, can be implanted in the knee. Once the stem cells grow and replace the missing cartilage, the printed tissue scaffolds would dissolve safely inside the body.

A bright future dotted with challenges
It is evident that medical electronics is part and parcel of our future. The rate at which folks in the industry and academia are innovating in this space, we might actually see implants being sold in medical shops and doctors printing devices on their desks.
However, some practical issues need to be sorted out before that. One, of course, is the well-known issue of battery life, a serious concern that limits the life of implants.
Several options are being explored to overcome this. While some are experimenting with wireless charging, others are working on off-beat options, such as a battery-less cardiac pacemaker developed at University of Bern, Switzerland. The pacemaker charges itself much on the lines of an automatic watch.
Another issue is security. In 2012, American TV show Homeland featured an episode in which terrorists hacked into the pacemaker of the US vice president and assassinated him. As readers stood aghast at the possibility, Forbes explored it and asserted that it is a real danger.
Around the same time, famous hacker Barnaby Jack and others like him demonstrated the possibility of hacking into medical devices like insulin pumps and pacemakers. While some companies revamped their devices after that, the danger still lurks as technical publications around the world continue to discuss this as a serious issue. Security features have to be made mandatory in medical devices, if patients are to have complete confidence in these.
In the years to come, these issues will hopefully be ironed out, so that the wonderful research by today’s labs can, so to say, win a place in people’s hearts!



This is quiet a good inovation especially for the rural areas like telemedicine