With the advances in science and technology, there has been a phenomenal growth in the use of electronic devices in the medical field. At present, various electrical devices are being engineered that could help patients recover from illness by replacing almost any disabled body part.
Science and technology are making great advances in all fields, particularly with the phenomenal growth of applications in various fields. The medical field has also embraced the use of electronic devices by not only helping patients recover from illness but also replacing medically stained/disabled human body parts, thus moving towards a complete electronics human body.
At present, various electrical and electronic devices are being engineered that can blend with the organs and tissues of the human body.
Some of the commonly used electronic devices at present are mediators, recorders, and stimulators of electricity, with the capacity to monitor important electrophysiological events, replace disabled body parts, or even stimulate tissues to overcome their limitations. The use of such electronic devices or organs in place of disabled human organs is capable of leading humans into the age of cyborgs.
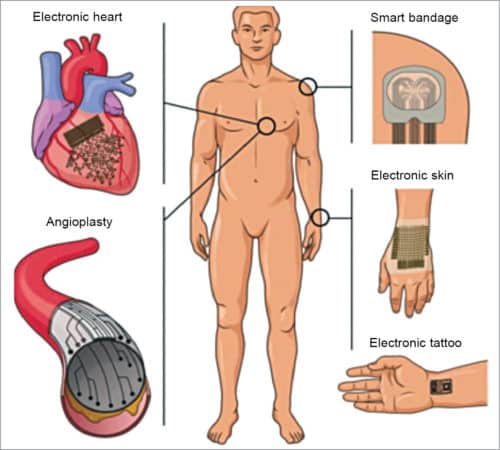
Further, such advances in electronic or artificial organs have been possible by the emergence of flexible and soft electronic materials that can readily integrate with the human body. An electronic organ is a device or tissue that is integrated into the human body—interfacing with living tissues—to replace a natural organ in order to duplicate or augment a specific function. This helps patients return to normal life as soon as possible. Use of artificial organ may help patients in the following ways:
- By providing life support to prevent imminent death while awaiting a treatment
- By improving the ability for self-care
- By improving the ability to interact socially
- By improving the quality of life
This article covers the importance of electronics in medical sciences with special emphasis on the development of electronic devices, which not only treat injuries and diseases but also help replace infected human organs. Modern electronic devices are being developed with the use of smart and multifunctional materials to satisfy the need for soft, curvilinear, and continuously evolving characteristics of the human body.
The resulting electronic devices with unique capabilities in biomedical research and clinical medicine can very well integrate onto or into the human body for diagnostics, therapeutic, or surgical functions with a strong potential to improve human health and enhance the understanding of living systems.
With all these developments, researchers are working on replacing every organ of the human body for long and healthy living. This article covers a brief history of developments related to different vital parts of a body like brain, skin, ear, eyes, nose, heart, liver, kidneys, hands, and legs.
However, electronic devices or implants may suffer electromagnetic interference, corrosion, and wear and tear with time. Also, due to repeated operations, these require batteries replacement. Therefore making corrosion-free and more durable electronic devices that can be powered using movement or other energy sources from the body could be the answer.
Human brain
Human brain is the most delicate and complicated organ that controls the functioning of the whole body. In case something goes wrong with the functioning of brain, doctors try to understand and repair it within some limits. Neural prostheses are a series of devices that can substitute motor, sensory, or cognitive modalities that might have been damaged as a result of an injury or disease.
Rather than replacing existing neural networks to restore function, these devices often serve by disrupting the output of existing malfunctioning nerve centres to eliminate symptoms. Scientists are working towards electronic brains. But brain is not just another organ as it contains all your thoughts and memories. So, a new electronic brain in the head may not be that beneficial. However, this hasn’t stopped scientists from growing actual human brains in a lab. Starting with nothing but stem cells, scientists have managed to create brains equivalent to those of nine-week-old fetuses.
These miniature brains are the size of peas and are incapable of thought so far. The one thing keeping the brains from growing beyond this stage and becoming fully functional is that they have no blood supply. Though these brains aren’t placed into anyone’s body, these are proving a great resource for scientists investigating brain diseases.
Electronic heart
Implantable cardiac defibrillator (ICD) is an electronic device that is placed inside the body to track heart rhythm. It sends a low-intensity shock to the heart muscle if the rhythm becomes abnormal. Some ICDs use a pacing system instead of a shock.
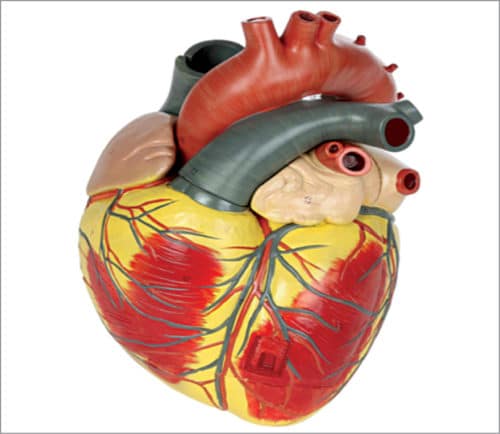
An artificial heart can completely replace a diseased heart and get blood pressure back to normal. While it isn’t meant to be a permanent replacement, it keeps people with heart failure alive until they receive an actual transplant. Cardiovascular-related artificial organs are implanted in cases where the heart, its valves, or another part of the circulatory system is not working properly.
Besides these, lab-grown and 3D-printed hearts are also being researched. Scientists have investigated stem cells’ potential, and they have reached a major milestone after creating heart tissue that can beat on its own.
Researchers used stem cells made from the skin to make MCP, a special kind of cell that acts as a precursor to cardiovascular tissue. It was then placed on a 3D scaffold designed to support a mouse heart. Within twenty days, the new heart began beating at forty to fifty beats per minute. Though this heart is too weak to actually pump blood, the tissue has a lot of potential for repairing heart muscles that have suffered damage.
Electronic skin
Skin protects the whole body, making it the most easily damaged organ. When the skin is burnt or rips off, the main option right now is to graft some back on from elsewhere on the body. But an effective synthetic replacement of skin may not be that far. Skin-like electronics that can adhere seamlessly to human skin or within the body are highly desirable for applications such as health monitoring, medical treatment, medical implants, and biological studies and for technologies that include human-machine interfaces, soft robotics, and augmented reality.
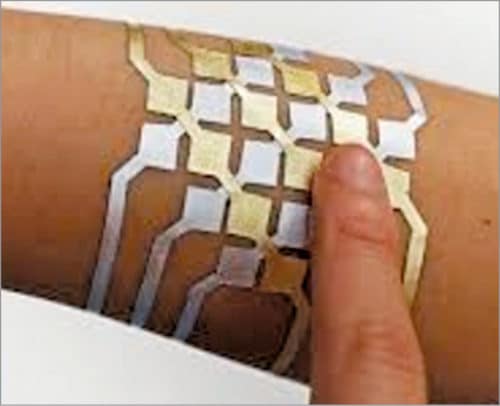
Rendering such electronics that are soft and stretchable like human skin would make them more comfortable to wear. Structural engineering of rigid inorganic and organic devices has enabled circuit-level stretchability, but this requires sophisticated fabrication techniques and usually suffers from reduced densities of devices within an array.
Scientists have developed a super-flexible, super-durable, and super-sensitive material that can be the basis for future synthetic skin. It contains organic transistors and a layer of elastic, letting it stretch without any damage. Further, it can also be self-powered as it can contain a series of elastic solar cells.
Artificial eyes
Medical science has been able to restore hearing, but restoring sight to the blind is much more complicated. When people lose their sight, their retinas no longer send signals from their photoreceptors to their brains. To make an artificial eye, it is important to understand how the retina processes those signals, and scientists haven’t been able to crack this yet.
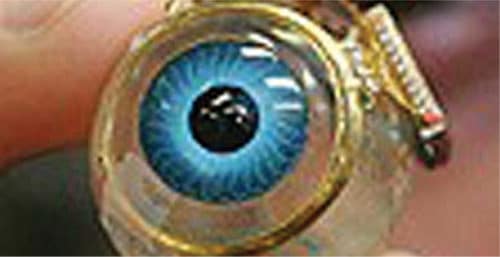
The artificial eye produces artificial retinas, whose chips convert images into electronic signals, and tiny projectors convert electronic signals into light. These artificial eyes have indeed restored sight to blind mice, and the follow-up experiments on monkeys offer hope for trials on humans.
The most successful function-replacing artificial eye so far is an external miniature digital camera with a remote unidirectional electronic interface implanted on the retina, optic nerve, or other related locations inside the brain. The present state-of-the-art yields only partial functionality, such as recognising levels of brightness, swatches of colour, and/or basic geometric shapes. No doubt, the problem of creating a completely functional artificial electronic eye is even more complex but advances towards tackling the complexity of the artificial connection to the retina, optic nerve, or related brain areas, combined with ongoing advances in computer science, are expected to dramatically improve the performance of this technology.
Printed ears
In cases when a person is profoundly deaf or severely hard of hearing in both ears, a cochlear implant may be surgically implanted. Cochlear implants bypass most of the peripheral auditory system to provide a sense of sound via a microphone and some electronics that reside outside the skin, generally behind the ear.
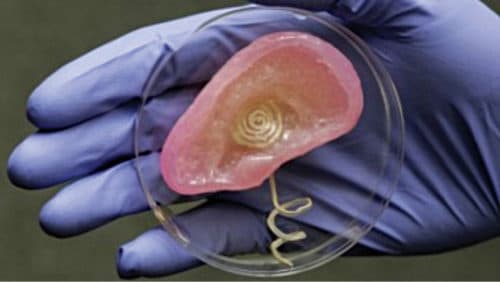
The external components transmit a signal to an array of electrodes placed in the cochlea, which in turn stimulates the cochlear nerve, but internal implants do nothing for the visible parts of the ear. Traditional replacements to ears look and feel like plastic toys. But recently, researchers have come up with a new method that makes flexible, realistic ears out of real cells. The artificial ear then just needs a few days to grow in nutrients before it’s ready to be implanted in a subject. Artificial ears will be a huge benefit to those who suffer injuries.
E-nose
Smells are composed of molecules, and each of these molecules has a corresponding sized and shaped receptor in the human nose. When a specific receptor receives a molecule, it sends a signal to brain. Brain identifies smell associated with a particular molecule.
An electronic nose is a device that detects smell more effectively than a human nose. An electronic nose consists of a mechanism for chemical detection. It is an intelligent sensing device that uses an array of gas sensors that are overlapping selectively along with a patterned reorganisation component.

Electronic noses work in a similar manner as a human nose. The electronic nose uses sensors as the receptor. When a specific sensor receives the molecules, it transmits the signal to a program for processing rather than to brain.
Nowadays, electronic noses provide several benefits to a variety of commercial industries, agriculture, biomedical, cosmetics, environmental, food, water, and various scientific research fields. The electronic nose detects hazardous or poisonous gas, which is not possible for human sniffers.
Hands with a sense of touch
Electronic hands have to accomplish the human hands’ most important ability—the sense of touch. Current prosthetic hands do little beyond filling the arm-shaped space between the body and air. People with prosthetics can’t detect if they’re in contact with an object without looking at it directly. A research team has solved this problem by inventing hands that send electric signals to brain.

When outfitted with prosthetic hands that stimulate the brain that way, monkeys responded just as though they physically touched objects themselves. Programming these same signals into artificial human limbs would give amputees replacement hands, unlike anything developed before.
Bionic arm and legs
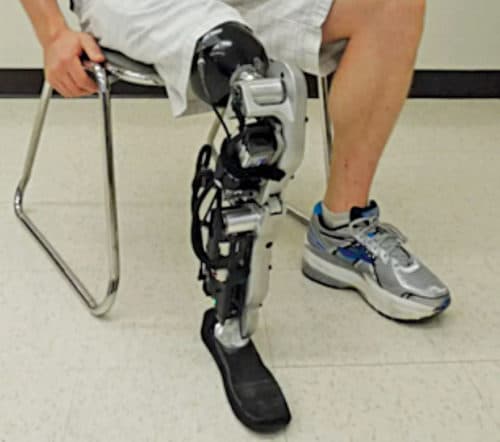
Artificial arms and legs, or prosthetics, are intended to restore a degree of normal function to amputees. Prosthetic arms have been around since ancient Greece, but a fully mechanised one—controlled entirely by the mind—wasn’t developed until recently.
Jesse Sullivan was the recipient of the world’s first brain-controlled bionic arms, installed through nerve transfer surgery and managed by a computer embedded in his forearm. New plastics and other materials, such as carbon fibre, have allowed artificial limbs to become stronger and lighter, limiting the amount of extra energy necessary to operate the limb and to look much more realistic.
Artificial pancreas
An artificial pancreas is used to substitute the endocrine functionality of a healthy pancreas for diabetic and other patients who require it. It can be used for insulin replacement therapy until glycemic control is practically normal as evidenced by the avoidance of complications of hyperglycemia. It can also ease the burden of therapy for insulin-dependent.
Artificial pancreas knocks insulin into the body automatically. The device looks much like a regular insulin pump, which slips insulin continuously through the skin. But this one monitors blood sugar at all times and adjusts itself accordingly. Unlike several electronic items for the human body, the artificial pancreas is still in early development stages.
Electronic bladder
Electrical stimulation is used to treat urinary incontinence by sending a mild electric current to nerves in the lower back or pelvic muscles that are involved in urination. The stimulation may make muscles contract, producing an effect that strengthens muscles by contracting these frequently. The stimulation may also encourage the growth of nerve cells that causes muscles to contract.
Electrical stimulation of the bladder can also be done by placing electrodes under the skin, either through legs or into the lower back. The two main methods for replacing the bladder function involve either redirecting urine flow or replacing the bladder in situ. The standard method for replacing the bladder involves forming a bladder-like pouch from intestinal tissue. Methods to grow bladders using stem cells have been attempted in clinical research.
Electronic liver
Scientists are developing a bioartificial liver device intended for the treatment of liver failure using stem cells. The artificial liver is designed to serve as a supportive device, either allowing the liver to regenerate upon failure or to bridge the patient’s liver functions until a transplant is available. Though it uses real liver cells, it is not a permanent substitute.
Researchers have found that a mixture of human liver precursor cells (differentiated from human induced pluripotent stem cells) and two other cell types can spontaneously form three-dimensional structures dubbed ‘liver buds.’
Electronic lungs
Artificial lungs promise to be a great success in the near future. A company is currently working on this type of medical device.
Extracorporeal membrane oxygenation (ECMO) can be used to take a significant load off of the native lung tissue and heart. In ECMO, one or more catheters are placed into a patient’s body, and a pump is used to flow blood over hollow membrane fibres, which exchange oxygen and carbon dioxide with the blood.
Similar to ECMO, Extracorporeal CO2 Removal (ECCO2R) has a similar set-up but mainly benefits a patient through carbon dioxide removal rather than oxygenation, allowing the lungs to relax and heal.
Dr S.S. Verma is professor at Department of Physics, Sant Longowal Institute of Engineering and Technology, Sangrur, Punjab





