The device improves the safety and effectiveness of spinal cord injury treatments, representing a step forward in therapy.
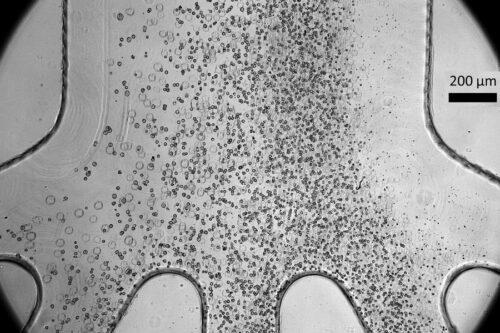
A compact device developed by researchers at MIT and the Singapore-MIT Alliance for Research and Technology can potentially enhance the safety and efficacy of cell therapy treatments for individuals with spinal cord injuries.
Researchers have developed a device that regenerates injured spinal cord parts but faces the challenge of undifferentiated stem cells potentially causing tumours. Their solution, a microfluidic cell sorter, efficiently separates potential tumour-causing cells from healthy progenitor cells without damage. This device sorts over 3 million cells per minute, and when multiple devices are linked, they can handle over 500 million cells per minute. This advancement and the low-cost production of the device’s plastic chip promise a safer and more scalable approach to cell therapy treatments.
Reducing risk
The research team found that pluripotent stem cells are typically larger than the progenitor cells they give rise to, a difference believed to stem from the fact that, before differentiation, a pluripotent stem cell’s nucleus is packed with numerous active genes. As the cell begins to differentiate into a cell with a specific function, it deactivates many of these genes, which are no longer necessary, leading to a significant reduction in the size of its nucleus. Taking advantage of this size disparity, the microfluidic device is designed to sort cells, effectively distinguishing between pluripotent stem cells and their smaller, differentiated progenitor counterparts.
Spiral sorting
The researchers optimised their cell sorter by using it twice—first at a low speed to separate larger from smaller cells, then at a high speed to refine the separation. This process, akin to a centrifuge but automated, effectively removes about 50% of the larger tumour-risk cells without manual intervention. Proven to exclude cells linked to higher tumour risk, this filter-free, low-cost device is scalable for mass production. After demonstrating its effectiveness on a small scale, the team is moving towards larger studies and animal models to assess the purified cells’ functionality in living organisms. This method promises to enhance cell therapy’s safety and efficacy by eliminating more non-differentiated cells.



