FEBRUARY 2012: As healthcare moves out of hospitals and becomes more integrated with peoples’ lives, medical devices are evolving from portable equipment to wearable devices that are meant to be used continuously for extended periods of time. These new devices present designers with many new challenges.
Infusion drug therapy
Medical devices that are worn on the body are not new. Most people are familiar with wearable products, such as nicotine patches and motion sickness patches. These devices laid the groundwork for a new generation of electronic products. One member of this new generation is the iontophoresis patch.
Iontophoresis uses electrical current to enable the infusion of a drug through the skin. The transdermal drug is ionised, dissolved in an aqueous solution and applied to an electrode in the patch. This specially formulated ionised compound can then be moved through the skin via direct current (DC) (refer Fig. 1). Most patches used today can be worn for anywhere from a few minutes to a few hours, depending on the drug and the condition being treated.
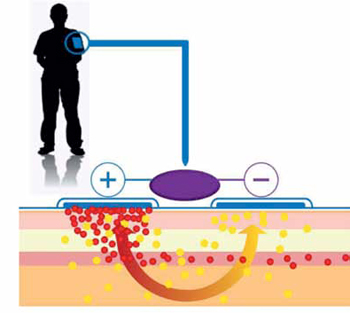
There are several advantages of iontophoresis. The medicine can be locally administered at very high levels rather than being distributed throughout the body, which happens with syringe injections. This local administration can result in improved efficacy and reduced side effects. Advances in electronics technology, such as switched-mode power sup ply design, along with cost-effective high-performance microcontrollers have made the production of low-cost single-use dispensers for these drugs possible. Self-applied iontophoresis has already been used by many consumers to deliver medicines for many conditions including headaches, cold sores and wrinkles.
One of the biggest challenges that designers face while creating devices such as iontophoresis patches is that critical electronics is in the wearable portion of the device, which is meant to be used once and then thrown away. This creates intense pressure for the patch electronics to be small and inexpensive. Also, since this is a small disposable item, battery cost and energy capacity impose further constraints on the design. Finally, the design needs to be easily modified for additional features such as changes in the medication dose and duration.
To infuse the drug through the skin, the device must produce sufficient voltages to drive the current level needed for the specific infusion dose rate, and for the required duration period. A working design for a small cost-sensitive iontophoresis device can be as simple as a DC-DC boost converter to drive a controlled current through the skin, along with a microcontroller to control the converter.
The boost regulator steps up the voltage from a low-voltage battery to sufficient levels for passing the required current through the skin. Inexpensive lithium coin or alkaline cell batteries can be used to provide power to patch electronics.
Meeting the requirements for both cost and functionality calls for a microcontroller that is small yet highly integrated. 8-pin, 8-bit microcontrollers are available for use in these devices. These meet the design integration requirement with an internal 10-bit analogue-to-digital converter, fixed voltage reference, comparator, pulse-width modulation, hardware timers and electrically erasable programmable read-only memory (EEPROM). The fixed voltage reference eliminates the need for a regulator or an external reference, and keeps the design to an 8-pin microcontroller in order to lower the cost and reduce board size.
Long-term monitoring
Long-term use of wearable medical devices is improving with innovations in electronics. Continuous glucose monitors and wearable cardiac-event recorders are examples of such devices.
A unique example of devices that take long-term use to a whole new level is the ovulation prediction system. These devices are used by women who want to maximise their chances of conceiving. One such wearable device is DuoFertility’s monitor (refer Fig. 2). This device made by Cambridge Temperature Concepts embodies a number of attributes that are essential to long-term monitoring systems in general.
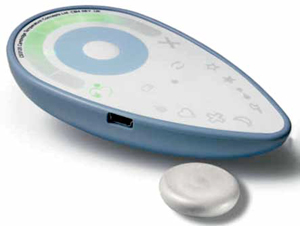
The ovulation process in a woman’s body correlates to minute changes in her basal body temperature. Accurately measuring those temperature changes over multiple monthly cycles can help to estimate the day of ovulation.
While a continuous glucose monitor may be designed to operate for up to a week, the sensor on this fertility device continuously measures body’s basal temperature for up to six months. The device uses this information to predict when ovulation will occur, up to six days in advance. Constantly monitoring minute temperature changes eliminates the many variations that occur in taking the temperature manually.





